
Introduction
We used to think of the gut as simple plumbing. Food went in, nutrients were absorbed, waste came out. But your digestive tract is considerably more interesting than that. It houses a complex microbial ecosystem that trains your immune system, regulates inflammation, and - through the gut-brain axis - influences your mood and energy.
70% of your immune system resides in your gut. Understanding why changes how you think about almost every chronic health problem.
In fact, gut health is one of the highest-impact areas we focus on when helping people build a foundation for long-term health.
The Gut Immune Connection
The gut is your body's primary interface with the outside world. Every meal introduces foreign substances, potential pathogens, and environmental compounds. The immune cells lining your gut wall have to make constant judgements: tolerate this, attack that.
This happens at the gut lining, where specialised immune cells continuously sample what passes through. Pattern recognition receptors detect microbial signals and determine the response - inflammation or tolerance. Get this balance right and your immune system functions precisely. Tip it the wrong way and you end up with a system that either under-responds to real threats or over-responds to harmless ones.
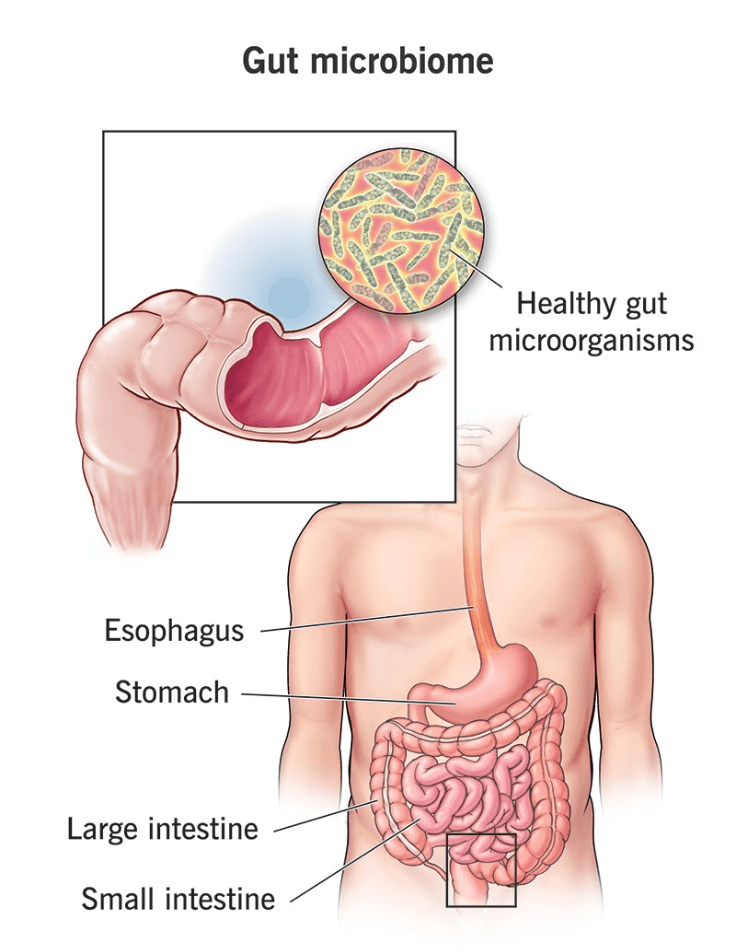
Image 1 - Gut Microbiome, Cleveland Clinic 2023
Gut Microbiota
Your gut microbiome - the collection of bacteria, viruses, and fungi in your digestive tract - is central to this process. A diverse, healthy microbiome does several things at once: it physically crowds out harmful bacteria, communicates directly with immune cells, and produces short-chain fatty acids (SCFAs) when it breaks down dietary fibre.
SCFAs are not a minor detail. They are the primary fuel for the cells lining your colon. They strengthen the gut barrier, reducing the risk of 'leaky gut' - a state in which microbial fragments and toxins pass into the bloodstream and trigger widespread inflammation. Adequate Vitamin D also supports this barrier function.
When the microbiome is disrupted - by infection, antibiotics, chronic stress, or a diet heavy in ultra-processed foods - this communication breaks down. The immune system loses its calibration. Overactivation can follow, where it begins attacking the body's own tissues. This is thought to be one pathway into autoimmune disease.
Discover the 5 habits that boost your longevity
Unlock a doctor-reviewed 5-day guide to the core pillars of long-term health—diet, exercise, lifestyle, sleep, and mental wellbeing. Evidence-based, practical, and designed to help you start making meaningful changes today.
No spam. Unsubscribe anytime.
By continuing, you agree to receive occasional updates from Emerald. See our Privacy Policy.
Chronic Inflammation
Acute inflammation heals a wound. Chronic inflammation, sustained over years at low intensity, damages tissues and drives disease - from cardiovascular problems to metabolic dysfunction.
Dysbiosis (an imbalance in gut bacteria, where harmful strains outnumber beneficial ones) is a significant driver of this state. When the gut barrier is compromised, bacterial toxins - particularly lipopolysaccharides (LPS) from gram-negative bacteria - can enter the bloodstream. The immune response this triggers is not localised. It circulates. Over time, this is one reason dysbiosis is associated with brain fog, persistent fatigue, and conditions that appear to have nothing to do with digestion.
This is why the Mediterranean diet and fermented foods carry real clinical weight. Whole grains and prebiotic-rich foods feed beneficial bacteria. Fermented foods like kefir and kimchi introduce live cultures that may help restore diversity. These are not lifestyle preferences - they are anti-inflammatory interventions with a reasonable evidence base.
One important caveat: you cannot out-supplement a poor diet. Probiotics have a role, but their benefits are modest and short-lived if the dietary environment they land in starves them out within weeks. The underlying diet matters more.
What Disrupts the Microbiome
Your gut is shaped by environment and behaviour in ways most people underestimate.
Stress alters gut motility and secretion, changing the conditions your microbes live in. This is the gut-brain axis in practice - and it's why stress so reliably produces digestive symptoms. How you manage stress long-term matters for gut health. Understanding the difference between stress resilience and stress tolerance is a useful starting point.
Antibiotics are necessary when infections require them, but they indiscriminately reduce microbial diversity. Recovery is slow without deliberate effort - increasing prebiotic fibre intake and fermented foods in the weeks following a course can help reseed what was lost.
Sleep deprivation disrupts the microbiome through circadian mechanisms. The gut has its own clock, and when your sleep is fragmented or insufficient, microbial composition shifts in ways that have been linked to increased inflammation. Improving sleep quality is not a soft recommendation - it is one of the more direct levers you have on gut health.
Longevity starts with awareness
Less than £1/day. Test 115+ biomarkers. Personalised plan and 1:1 GP support.
What You Can Do
The practical case for gut health is straightforward: a diverse, well-fed microbiome reduces chronic inflammation, supports immune precision, and protects the gut barrier. Here is where to focus.
Eat more fibre, and vary the sources. Gut bacteria are selective feeders. Different strains thrive on different substrates. Thirty or more distinct plant foods per week - vegetables, fruits, legumes, whole grains, nuts, seeds - has been associated with greater microbial diversity than eating fewer varieties, even if total fibre intake is similar.
Include fermented foods regularly. Kefir, natural yoghurt, kimchi, sauerkraut, and miso introduce live cultures and have been shown in randomised trials to increase microbial diversity and reduce markers of inflammation.
Limit ultra-processed foods. They are low in fibre, often high in emulsifiers that may disrupt the gut lining, and consistently associated with reduced microbial diversity in observational studies.
Manage stress actively. Not because it is pleasant to do so, but because the gut-brain axis is real and the downstream effects on the microbiome are measurable.
Treat antibiotics as a disruption that needs recovery. If you need a course, plan the dietary response.
Related articles
Test 115+ biomarkers for fine-tuning your health
See your results in 3 days with high-level accuracy and a certified GP-reviewed action plan




